NHS Crisis Warning: UK Ranked Among Worst for Avoidable Deaths in Global Health League Table
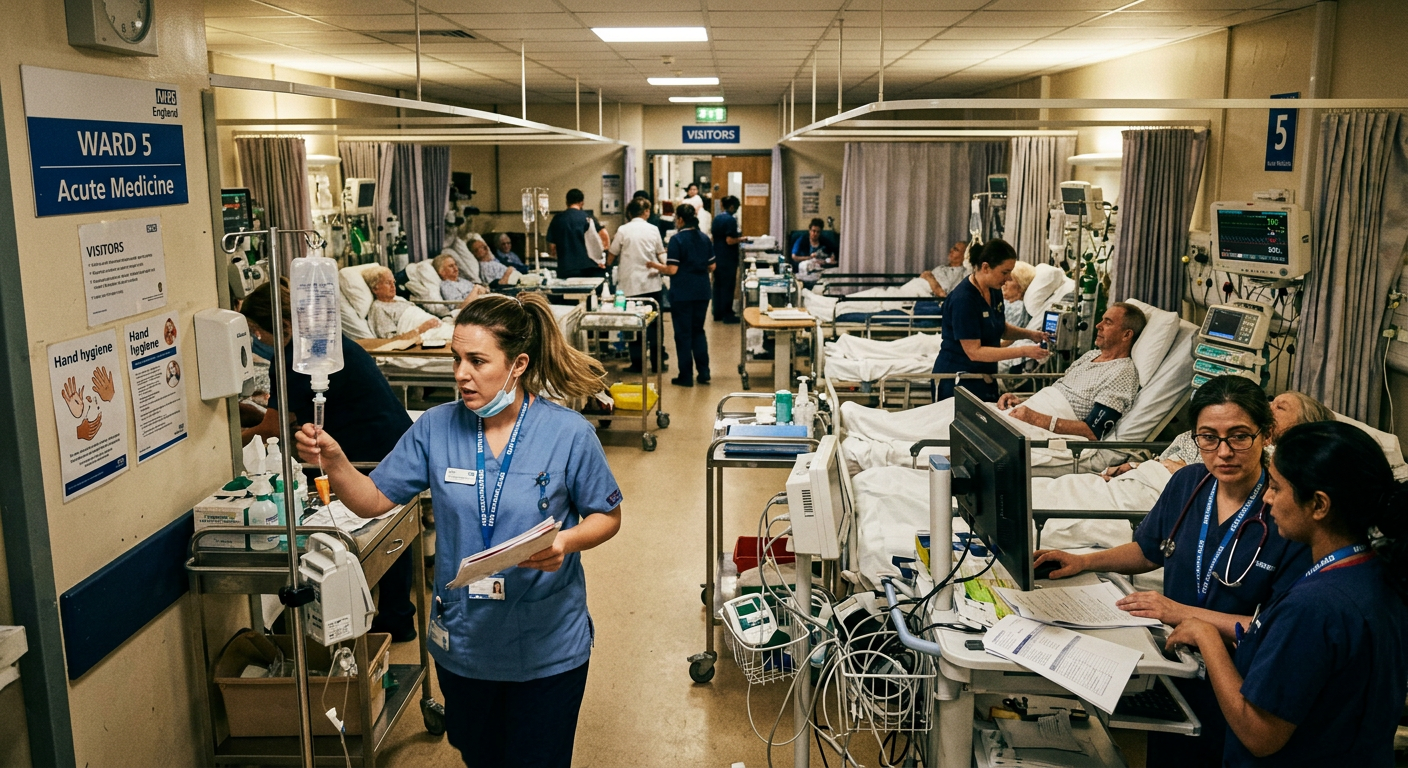
The latest NHS news has delivered a stark warning about the state of healthcare in the UK, as a new international report reveals the NHS ranks among the worst-performing systems for avoidable deaths in the developed world.
According to the analysis, the UK now sits second from bottom in a league table of 22 developed nations measuring “treatable mortality”—deaths that could have been prevented with timely and effective medical care. Only the United States ranked lower, raising serious concerns about NHS performance, patient outcomes, and healthcare access in the UK.
The report, published by the Institute for Public Policy Research (IPPR), highlights years of underinvestment and poor allocation of resources as key drivers behind the NHS’s struggles. While overall health spending has increased significantly—rising by more than £60 billion over the past decade—experts argue that the money has not been spent where it is most needed.
Instead of investing heavily in infrastructure such as hospital buildings, diagnostic equipment, and modern technology, much of the funding has been directed towards staffing and pay. As a result, the UK now lags comparable countries in basic healthcare capacity, with fewer hospital beds and significantly less access to essential diagnostic tools.
The figures paint a concerning picture. The UK currently has just 19 MRI, CT, and PET scanners per million people, compared to around 50 in countries like Sweden, Spain, and Australia. In nations with social insurance-based healthcare systems, such as Switzerland and France, this number rises to an average of 68 scanners per million. This lack of equipment is contributing to long NHS waiting times, delayed diagnoses, and reduced survival rates.
Experts say these shortages are having a direct impact on patient outcomes. The UK performs below average in key indicators such as survival rates within 30 days of a heart attack—one of the most critical measures of healthcare effectiveness. Limited capacity and delays in treatment are believed to be major contributing factors.
Despite growing debate around whether the UK should adopt a European-style insurance-based healthcare system, the IPPR firmly rejects the idea. Analysts argue that switching models would not solve the NHS’s core problems and could instead distract from the real issue: how resources are allocated.
Healthcare leaders are calling for urgent action, including increased investment in NHS infrastructure, improved access to diagnostic services, and a stronger focus on community-based care. Addressing pressures in social care is also seen as essential to reducing unnecessary hospital admissions and easing strain on the system.
Health Secretary Wes Streeting acknowledged the challenges but defended the NHS model, emphasising that the priority must be ensuring funding is used effectively. He reiterated that the founding principle of the NHS—providing healthcare based on need rather than ability to pay—remains as important today as ever.
As pressure mounts, this report serves as a wake-up call. Without targeted investment and strategic reform, experts warn that the UK risks falling further behind in global health outcomes. For patients, the message is clear: improving NHS efficiency, reducing waiting times, and strengthening healthcare infrastructure must now become urgent national priorities.

